TL;DR:
- Foot pain is often ignored but can lead to serious issues if untreated, making podiatric care essential. Most foot conditions, including heel pain and deformities, respond well to conservative treatments like orthotics and physical therapy, reserving surgery for persistent cases. Regular follow-up is especially vital for high-risk patients with diabetes or circulation problems to prevent severe complications.
Foot pain is one of the most commonly ignored health signals in the body. Many people assume that soreness, stiffness, or even sharp pain in the feet is just part of staying active, getting older, or standing on hard floors all day. But dismissing foot discomfort can quietly set the stage for serious problems, including chronic injury, nerve damage, and in high-risk patients, limb loss. This guide walks you through exactly why podiatric care matters, what to expect from your first visit, how most conditions are treated without surgery, and how to choose the right specialist when you need one in Las Vegas.
Table of Contents
- What does a podiatrist do—and who should consider seeing one?
- Conservative treatments vs. foot surgery: What you should know
- Why follow-up care matters, especially for high-risk feet
- Podiatrist or orthopedist? Choosing the right specialist in Las Vegas
- A podiatrist’s perspective: What most people miss about foot care
- Ready to take the next step? Expert podiatry care in Las Vegas
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Specialist expertise | Podiatrists offer focused diagnosis and solutions for all foot and ankle problems. |
| Conservative care first | Most foot pain, including heel pain, responds well to non-surgical treatments. |
| Diabetic foot outcomes | Ongoing podiatric follow-up significantly lowers the risk of amputation. |
| Choosing the right provider | Foot/ankle-centered pain is usually best started with a podiatrist. |
| Early intervention | Addressing issues sooner with expert care prevents chronic problems and surgery. |
What does a podiatrist do—and who should consider seeing one?
A podiatrist is a doctor of podiatric medicine (DPM) who specializes exclusively in diagnosing and treating conditions affecting the foot, ankle, and lower leg. Unlike a general practitioner who might glance at a swollen ankle and recommend rest, a podiatrist brings years of specialty training in biomechanics, wound care, nail and skin disorders, surgical intervention, and chronic disease management. Think of them as the go-to expert when everything from the knee down isn’t working the way it should.
Many patients visit a podiatrist for general foot & ankle care that ranges from ingrown toenail treatment to complex reconstruction. Others come in after months of pain that their primary care doctor couldn’t fully resolve. Both approaches make sense, but one is almost always faster and more effective than the other.
Common reasons to see a podiatrist
If you’re wondering whether your situation warrants a specialist visit, here are the most frequent scenarios where podiatric care makes a clear difference:
- Persistent heel pain or arch pain that doesn’t improve after a week or two of rest
- Foot or ankle injuries, including sprains, stress fractures, and tendon tears
- Diabetes, since nerve damage and poor circulation make even small wounds dangerous
- Skin and nail problems, including fungal infections, corns, calluses, and warts
- Bunions or hammertoes that are causing pain or changing how you walk
- Numbness, tingling, or burning in the feet, which may signal nerve involvement
- Changes in gait or uneven shoe wear that suggest a structural issue
- Wounds or ulcers that aren’t healing, especially in patients with diabetes or vascular disease
Waiting for these symptoms to resolve on their own is one of the most common and costly mistakes patients make. Research has shown that podiatric follow-up improves outcomes in patients with diabetic foot disease, with evidence linking specialty care to better limb survival and reduced mortality. That’s not a minor benefit. That’s a life-changing one.
Pro Tip: If you’re unsure whether your foot problem needs a specialist, err on the side of getting it checked. A podiatrist can usually rule out serious causes quickly, and what to look for in a foot doctor matters as much as getting there promptly.
| Symptom or condition | Why a podiatrist is the right call |
|---|---|
| Heel pain lasting more than 2 weeks | May indicate plantar fasciitis or nerve entrapment |
| Diabetic foot wound | Risk of infection, ulcer, or amputation without specialty management |
| Nail or skin changes | Could be fungal, bacterial, or a sign of systemic disease |
| Ankle instability after a sprain | Incomplete healing increases re-injury risk |
| Bunion or structural deformity | Biomechanical issues worsen without proper assessment |
| Pain that changes how you walk | Compensation patterns create new injuries up the chain |
The idea that foot pain is just a “normal” part of daily life has no clinical basis. Persistent pain is your body’s way of asking for help. Taking that signal seriously, and acting on it early, is precisely what separates patients who recover fully from those who manage a nagging problem for years. Learning about foot injury prevention tips is a great first step before symptoms become something harder to treat.
Conservative treatments vs. foot surgery: What you should know
Once you’ve decided to see a podiatrist, the next natural question is: will I need surgery? For most patients, the answer is no. The vast majority of foot and ankle conditions respond well to non-surgical care when it’s started early and followed consistently.
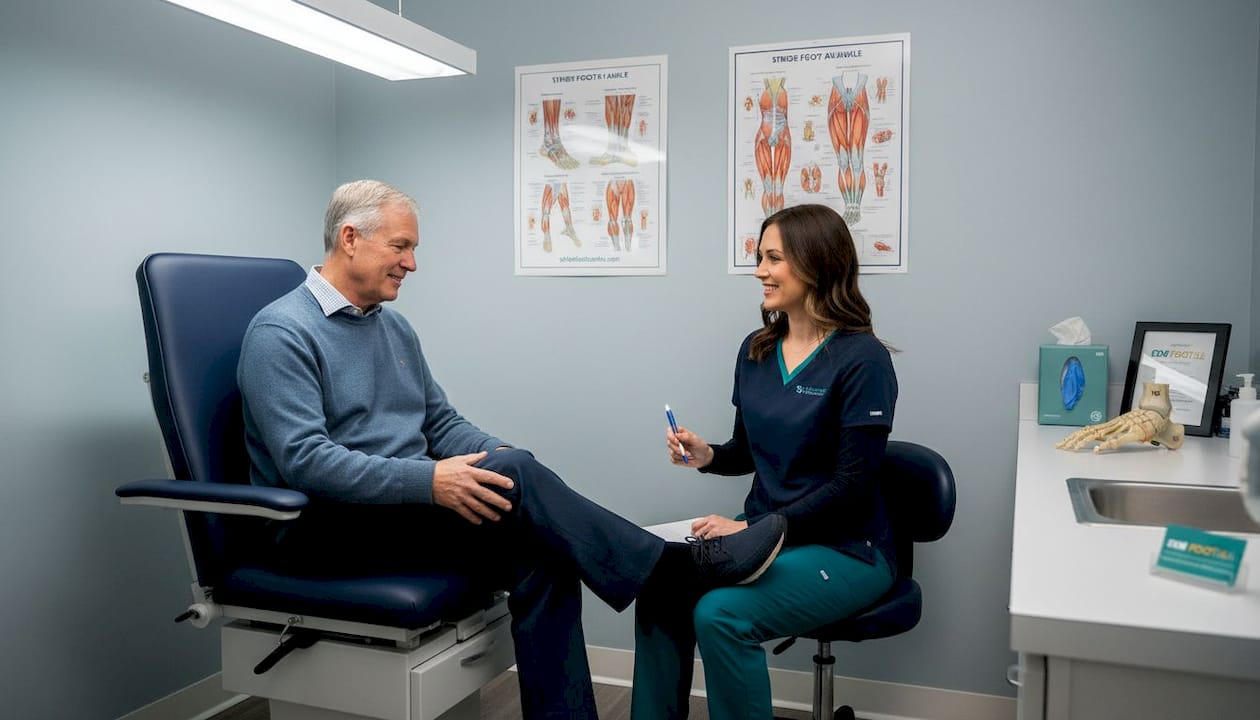
For one of the most common complaints, heel pain caused by plantar fasciitis (inflammation of the thick band of tissue connecting the heel bone to the toes), conservative treatment resolves most cases without any surgical intervention. Clinical guidelines recommend trying conservative methods for at least 6 to 12 months before surgery is considered. That’s not a delay tactic. It’s evidence-based medicine.
What conservative foot care includes
Conservative foot care covers a range of targeted, non-invasive treatments. These aren’t just “wait and see” approaches. They’re active, structured protocols designed to reduce pain, restore function, and prevent recurrence.
Common conservative treatments include:
- Custom orthotics, which are shoe inserts molded to your foot to correct biomechanical imbalances
- Physical therapy with targeted stretching and strengthening exercises for the plantar fascia and Achilles tendon
- Night splints that keep the foot in a gentle stretch overnight to reduce morning pain
- Corticosteroid injections for acute inflammation that isn’t responding to rest and physical therapy
- Immobilization with a walking boot for stress fractures or severe tendon irritation
- Anti-inflammatory medications to reduce pain and swelling in the short term
- Activity modification and shoe recommendations tailored to your foot structure
The step-by-step approach to managing foot pain
- Initial assessment by a podiatrist to diagnose the root cause, not just the symptoms
- Start conservative care with targeted stretching, footwear changes, and activity adjustments
- Add orthotics or bracing if initial measures don’t produce improvement within 4 to 6 weeks
- Consider physical therapy for cases with muscle weakness or movement dysfunction
- Evaluate with imaging (X-ray, ultrasound, or MRI) if symptoms persist or worsen
- Discuss injection therapy for conditions with significant, localized inflammation
- Reassess at 6 to 12 months before considering any surgical option
| Approach | Pros | Cons | Typical recovery |
|---|---|---|---|
| Conservative care | Non-invasive, lower risk, no downtime | May take weeks to months for full relief | Weeks to a few months |
| Minimally invasive surgery | Smaller incisions, less tissue disruption, faster recovery | Still requires healing time and follow-up | 4 to 8 weeks |
| Traditional open surgery | Effective for complex or severe deformities | Longer recovery, greater surgical risk | 2 to 6 months |
If symptoms persist despite thorough conservative management, surgical options are available. Modern techniques have improved significantly. Minimally invasive foot surgery uses smaller incisions, causes less trauma to surrounding tissue, and typically shortens recovery time compared to traditional open procedures. For patients who do reach that stage, knowing how to prepare makes a real difference, and understanding the steps involved in preparing for foot surgery helps set realistic expectations for what comes next.
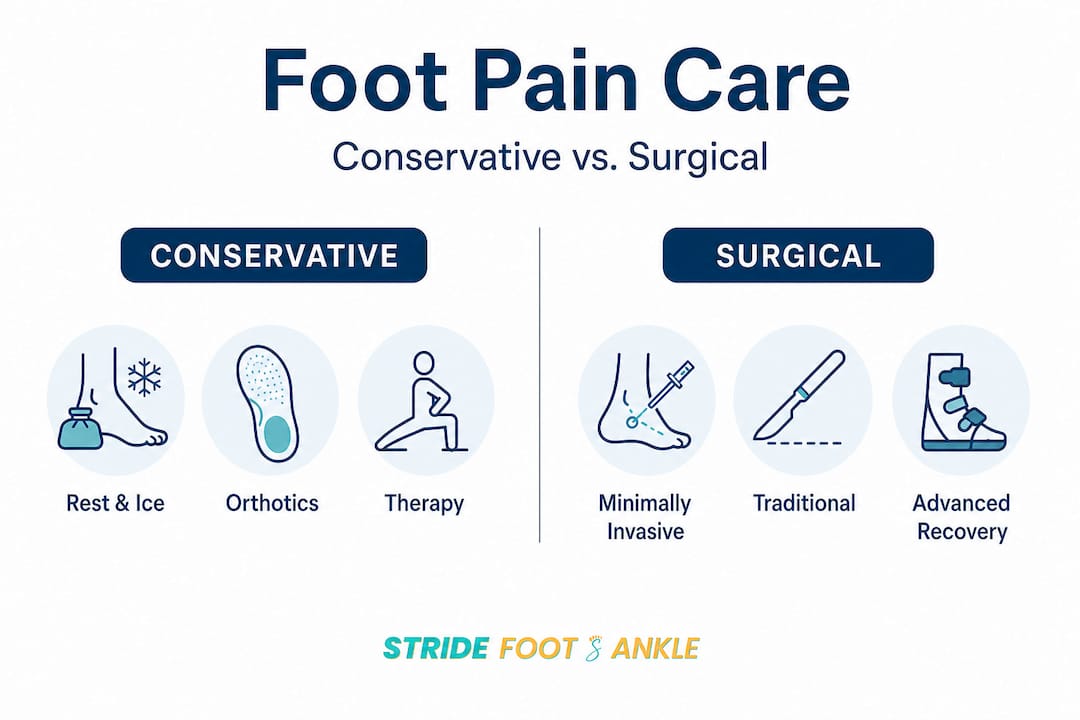
The takeaway here is straightforward: surgery is not the default. It’s a carefully considered option reserved for cases where months of evidence-based, nonsurgical care hasn’t produced the improvement you deserve.
Why follow-up care matters, especially for high-risk feet
Getting treatment is step one. Sticking with follow-up care is what makes treatment actually work, especially if you’re in a high-risk category. High-risk patients include anyone with:
- Diabetes, which can cause peripheral neuropathy (loss of feeling in the feet) and poor wound healing
- Peripheral arterial disease (PAD), which restricts blood flow to the lower extremities
- A history of foot ulcers, which dramatically increases the risk of recurrence
- Immune suppression from medications or chronic conditions
- Previous partial amputation, which changes how weight is distributed across the foot
For these groups, a missed follow-up appointment isn’t just an inconvenience. It can be the difference between catching a developing wound early and facing a serious infection. Data shows that ongoing podiatric specialty care is associated with better limb and survival outcomes in patients with diabetic foot disease. That evidence directly challenges the idea that follow-up visits are optional once initial treatment is done.
“Some podiatry follow-up is associated with better limb and survival outcomes in patients with diabetic foot disease, suggesting potential value in ongoing specialty care for high-risk feet.” (MDPI, 2024)
What a podiatric follow-up visit actually covers
Follow-up care with a podiatrist is thorough and proactive. It isn’t just checking in. A typical visit for a high-risk patient may include:
- Skin and nail inspection to catch early signs of infection, pressure sores, or nail disease
- Neurological assessment using a monofilament or tuning fork to check for sensation loss
- Vascular assessment to evaluate blood flow to the foot
- Wound measurement and documentation if an ulcer is present
- Footwear review to ensure shoes aren’t creating new pressure points
- Patient education on daily foot inspection techniques and warning signs
For patients managing diabetes, finding appropriate foot care products for diabetes between appointments is one practical way to stay proactive at home. But no product replaces clinical oversight.
| Care scenario | Likely outcome with follow-up | Likely outcome without follow-up |
|---|---|---|
| Diabetic patient with early ulcer | Wound managed before infection sets in | Risk of infection, osteomyelitis (bone infection), amputation |
| Post-surgical foot care | Healing monitored, complications caught early | Increased risk of delayed healing or re-injury |
| Neuropathy patient with shoe irritation | Identified and corrected before skin breaks down | Undetected wound develops into ulcer |
| Patient with history of foot fracture | Gait and bone alignment maintained | Compensation patterns lead to new injury |
The pattern is consistent: regular follow-up keeps small problems small. Skipping it turns manageable issues into crises. For Las Vegas residents managing diabetes or chronic foot conditions, scheduling consistent appointments isn’t overcaution. It’s smart, proactive healthcare.
Podiatrist or orthopedist? Choosing the right specialist in Las Vegas
This is one of the questions we hear most often, and it’s a fair one. Both podiatrists and orthopedists treat conditions involving bones, joints, and soft tissue. The difference lies in focus and training.
A podiatrist spends their entire medical education and residency training on the foot, ankle, and lower leg. They handle surgical and nonsurgical care, including chronic disease management unique to the foot, such as diabetic complications, nail disorders, and skin conditions. An orthopedic surgeon, by contrast, covers the entire musculoskeletal system, from the spine to the shoulders to the knees, and may specialize further in a subspecialty like sports medicine or joint replacement.
There’s real overlap in the foot and ankle space. Both specialists can perform surgery on the ankle, address fractures, and manage tendon injuries. As guidance from medical education sources notes, podiatry and orthopedics overlap in the foot and ankle, and the best starting point depends on where the pain is centered.
Pro Tip: If your pain starts in the foot or ankle and doesn’t radiate up the leg, a podiatrist is usually the most efficient first stop. They can diagnose and treat the full range of foot conditions without requiring a referral pathway through orthopedics.
| Condition or symptom | Best starting specialist |
|---|---|
| Heel pain, plantar fasciitis | Podiatrist |
| Bunions or hammertoes | Podiatrist |
| Diabetic foot wound or ulcer | Podiatrist |
| Ingrown toenails, fungal nails | Podiatrist |
| Ankle fracture or ligament tear | Either (podiatrist for isolated ankle injury) |
| Knee pain radiating down the leg | Orthopedist |
| Hip or back pain with leg symptoms | Orthopedist |
| Complex trauma involving multiple joints | Orthopedist or trauma surgeon |
When to see each type of specialist
See a podiatrist when:
- Pain or injury is localized to the foot or ankle
- You have diabetes, neuropathy, or a wound that isn’t healing
- You need skin, nail, or soft tissue care specific to the foot
- You want a specialist who focuses entirely on the lower extremity
See an orthopedist when:
- Your symptoms involve the knee, hip, or spine in addition to the foot
- You’ve had a traumatic injury involving multiple areas
- You need joint replacement surgery for larger joints
For Las Vegas residents navigating this choice, choosing the right podiatrist involves looking at credentials, surgical training, and whether the practice offers both conservative and advanced treatment options. Having both under one roof is a significant advantage.
A podiatrist’s perspective: What most people miss about foot care
We see patterns every day in practice that most general health articles don’t address directly. Here’s the honest truth about what makes a real difference for patients.
The most preventable outcome we encounter is the patient who waited too long. Someone who had mild heel pain for six months, tried stretching videos and drugstore insoles, then finally came in when the pain became constant. By that point, what might have resolved in six weeks of targeted care now requires a longer, more intensive treatment plan. The window for the simplest fix often closes quietly.
Home remedies and over-the-counter solutions aren’t inherently bad. Ice, rest, and supportive footwear have real value. But they work best as a bridge to proper care, not a substitute for it. A generic arch support from a pharmacy cannot replicate what a custom orthotic does for your specific foot structure. Anti-inflammatory gel might reduce pain today without addressing why the inflammation keeps coming back.
What we’ve observed specifically in Las Vegas patients is worth noting. The climate here is harsh on feet. Heat accelerates swelling. Hard surfaces in casinos, warehouses, and retail environments create relentless ground reaction forces. Many residents also walk significant distances in footwear chosen for appearance rather than function. These factors combine to create a higher background level of foot stress that makes early intervention even more valuable here than in other regions.
The surprising truth about prompt care is this: patients who come in early almost always need fewer appointments, fewer procedures, and experience less total downtime. The idea that seeing a doctor is a big deal you save for serious problems is backwards when it comes to the feet. Feet carry your entire body weight every single day. They deserve the same attention you’d give a car that started making a strange noise.
Connecting with a patient-centered podiatry perspective means finding a practice that treats you as a whole person, not just a symptom to be resolved. The best outcomes happen when patients understand their condition, trust their care plan, and feel empowered to ask questions and stay engaged with follow-up.
Trust your feet’s signals. They’re remarkably good at telling you when something is wrong. Acting on that signal early often means fewer appointments, less downtime, and a better outcome than you’d expect.
Ready to take the next step? Expert podiatry care in Las Vegas
Foot pain doesn’t have to slow you down or become a permanent part of your life. Whether you’re dealing with a nagging injury, managing a chronic condition like diabetes, or simply noticing changes in your feet that don’t feel right, expert podiatric care is available right here in Las Vegas.
At Stride Foot & Ankle, Dr. Nahad Wassel provides comprehensive podiatric services built around your individual needs, from general foot & ankle care and conservative treatments to advanced surgical options for complex conditions. If you’re facing the possibility of a procedure, guidance on preparing for foot surgery will help you feel informed and confident going in. And if you’re managing a wound or skin condition that isn’t healing, Stride Foot & Ankle offers ultrasound wound healing therapy, a specialized technology not widely available in the area. Book your appointment today and start striding confidently again.
Frequently asked questions
When should you see a podiatrist instead of your primary doctor for foot pain?
If foot pain is persistent, severe, or interfering with your daily activities, or if you have diabetes or a history of foot wounds, a podiatrist provides the specialized diagnosis and treatment that general practitioners aren’t trained to deliver.
How long should I try home treatments before seeing a podiatrist for heel pain?
While some improvement may occur with rest and stretching, guidelines recommend formal conservative care for at least 6 months before surgery is considered, but earlier evaluation often prevents the problem from becoming a longer-term issue.
Does seeing a podiatrist reduce the risk of foot amputation if you have diabetes?
Yes. Ongoing podiatric specialty care is directly associated with better limb and survival outcomes in patients with diabetic foot disease, making regular follow-up appointments one of the most important steps a diabetic patient can take.
Is surgery always the best option for chronic foot pain?
No. The vast majority of foot conditions, including plantar fasciitis, tendonitis, and many structural issues, improve with thorough conservative care. According to plantar fasciitis treatment guidelines, surgery is only considered after months of non-surgical treatment haven’t produced sufficient relief.
Recommended
- How to prevent foot injuries: expert strategies for healthy feet – Stride Foot & Ankle – Dr. Nahad Wassel
- Blog – Stride Foot & Ankle – Dr. Nahad Wassel
- Best Podiatrist Las Vegas: How to Choose the Right Foot and Ankle Specialist – Stride Foot & Ankle – Dr. Nahad Wassel
- General Foot & Ankle Care – Stride Foot & Ankle
Recent Comments