TL;DR:
- Minimally invasive foot surgery offers effective correction of deformities with less downtime and scarring. It is suitable for conditions like bunions and hammertoes but may not be ideal for severe cases requiring extensive correction. Choosing an experienced surgeon who evaluates your specific needs ensures optimal outcomes and long-term foot health.
Foot surgery has a reputation that scares many patients away from getting the care they actually need. Images of large incisions, months in a cast, and weeks on crutches make people put off treatment until the pain becomes unbearable. But that picture no longer tells the full story. Minimally invasive foot surgery (MIS) has changed what is possible, and Las Vegas patients now have access to techniques that deliver real results with far less downtime. If you have been living with bunions, hammertoes, or persistent foot pain, understanding MIS could be the turning point in your care journey.
Table of Contents
- What is minimally invasive foot surgery?
- Benefits and outcomes of minimally invasive foot surgery
- Common minimally invasive foot procedures in Las Vegas
- How to decide: Is minimally invasive surgery right for you?
- Our take: Why minimally invasive isn’t always the best choice
- Connect with experienced podiatrists in Las Vegas
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Quicker recovery | Minimally invasive foot surgery often leads to faster rehabilitation and less pain compared to traditional methods. |
| Evidence-based results | Clinical studies show lower pain scores and improved mobility after minimally invasive procedures. |
| Las Vegas expertise | Local podiatrists specialize in MIS, making advanced treatments accessible for most patients. |
| Not for everyone | Severe deformities or complicated cases may still require traditional, open surgery. |
| Consult wisely | Discuss goals, history, and options thoroughly with your podiatrist to determine the best approach. |
What is minimally invasive foot surgery?
Minimally invasive foot surgery is a modern surgical approach that uses very small incisions, often just a few millimeters wide, along with specialized tools and real-time imaging to correct foot conditions. Instead of opening up a large area of the foot, the surgeon works through tiny portals, causing far less disruption to the surrounding soft tissue, tendons, and nerves. The result is a procedure that achieves the same corrective goals as traditional open surgery but with a smaller wound and a gentler impact on the body overall.
Traditional open foot surgery requires cutting through layers of skin and soft tissue to access the bone or structure being treated. With MIS, surgeons use fluoroscopy (a type of real-time X-ray imaging) to guide their instruments precisely. This level of accuracy means less guesswork, more control, and ultimately a cleaner procedure. It is important to understand that MIS is not a shortcut. It demands advanced training and significant clinical experience to perform correctly.
Conditions commonly treated with MIS
Surgeons use minimally invasive techniques to address a wide variety of foot conditions. Here are the most frequently treated:
- Bunions (hallux valgus): The bony bump that forms at the base of the big toe, often pushing the toe out of alignment
- Hammertoes: A deformity where one or more toes bend abnormally at the middle joint, causing pain and difficulty wearing shoes
- Plantar fasciitis: Inflammation of the thick band of tissue running along the bottom of the foot, causing sharp heel pain
- Neuromas: Thickened nerve tissue that forms between the toes, usually between the third and fourth toe
- Bone spurs: Calcium deposits that grow on the edges of bones and cause friction and pain
Clinical evidence strongly backs up the effectiveness of MIS. In a study of 493 hallux valgus cases treated with a minimally invasive transverse osteotomy (MITA), the hallux valgus angle (HVA, the degree of big toe misalignment) improved from 34.24 degrees to 8.38 degrees, and the intermetatarsal angle (IMA, the gap between the first and second metatarsal bones) dropped from 12.67 to 5.78. Pain scores on the visual analog scale (VAS) fell from 2.91 to 0.20, and function scores on the American Orthopaedic Foot and Ankle Society (AOFAS) scale climbed from 82.20 to 99.11. These are not marginal improvements. They represent near-complete correction for the vast majority of patients.
For patients in Las Vegas exploring their options, learning about general foot and ankle care provides a solid foundation before deciding on any surgical approach. The foot surgery blog at Stride Foot and Ankle also offers updated, practical information on procedures and recovery timelines.
Benefits and outcomes of minimally invasive foot surgery
The numbers from MIS research are impressive, but what do they actually mean for your daily life? Let’s translate the clinical data into something you can feel and understand.
Pain reduction and functional improvement
The most immediate benefit most patients notice is pain relief. Using the VAS scale, where 10 is excruciating pain and 0 is none, post-MIS pain scores drop by more than two full points on average, with hallux valgus cases dropping nearly to zero. That kind of relief is life-changing for someone who has been modifying every step they take just to get through the day.

Functional outcomes are equally strong. The AOFAS scoring system grades foot function on a scale of 0 to 100. A rise of more than 15 to 20 points is considered clinically significant. The MIS studies reviewed showed an average improvement of nearly 17 points, putting most patients firmly in the “good” to “excellent” category post-surgery.
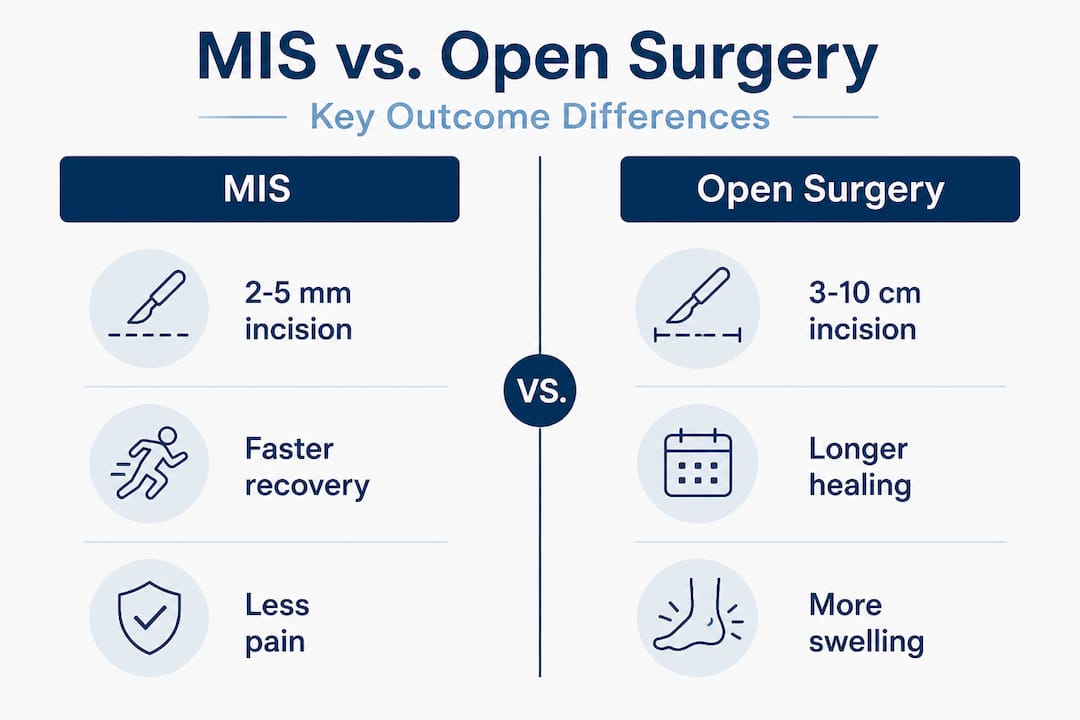
How MIS compares to traditional open surgery
| Feature | Minimally invasive surgery | Traditional open surgery |
|---|---|---|
| Incision size | 2 to 5 mm | 3 to 10 cm |
| Tissue disruption | Minimal | Moderate to significant |
| Average hospital stay | Outpatient (same day) | Overnight or longer |
| Initial recovery time | 2 to 6 weeks | 6 to 12 weeks |
| Scarring | Very minimal | Visible scar likely |
| Risk of infection | Lower | Slightly higher |
| Suitable for severe deformities | Limited | Yes |
| Use of imaging during procedure | Fluoroscopy required | Optional |
The comparison makes one thing clear: MIS wins on most quality-of-life metrics for eligible patients. However, the last row in the table is critical. Severe deformities often need the full visibility and access that only open surgery provides. Choosing MIS when open surgery is actually indicated can lead to incomplete correction and eventual revision surgery, which is far more difficult for everyone involved.
Additional benefits worth knowing
Beyond the numbers, MIS offers several practical advantages that improve the overall patient experience:
- Less postoperative swelling, which means less discomfort and faster return to wearing regular shoes
- Reduced risk of neurapraxia (temporary nerve irritation), which in MIS studies occurred in only about 6% of cases, mostly resolving on its own
- Lower anesthesia exposure, since shorter procedures often require less sedation
- Earlier weight-bearing, allowing many patients to walk in a protective boot within days instead of weeks
- Reduced scarring, which matters particularly to patients concerned about the cosmetic outcome
For patients who want to avoid surgery entirely or delay it while managing symptoms, nonsurgical tendon and ligament care is a worthwhile option to explore first. Your specialist can help you decide whether conservative treatment should come before or alongside surgical planning.
Pro Tip: If you are researching surgeons, look for practitioners listed among the top Las Vegas foot doctors who have formal training in MIS techniques specifically, not just general podiatric surgery. The difference in outcomes between a trained MIS specialist and a general podiatrist attempting the technique can be significant.
Common minimally invasive foot procedures in Las Vegas
Las Vegas has developed a strong community of podiatric specialists offering MIS, and patients here benefit from both high surgical volume and competitive standards of care. Here are the procedures most commonly performed using minimally invasive techniques in the area.
Top MIS procedures performed locally
Minimally invasive bunionectomy: Corrects hallux valgus deformity by realigning the first metatarsal bone through tiny incisions. This is the most commonly performed MIS foot procedure in Las Vegas and has the strongest body of clinical evidence supporting it.
Hammertoe correction: A small incision allows the surgeon to release or transfer tendons and reshape the affected toe joint. Patients typically return to wearing normal shoes within four to six weeks.
Plantar fascia release: For patients with severe plantar fasciitis that has not responded to conservative care, a small release of the tight plantar fascia (the band of tissue causing heel pain) can provide lasting relief.
Minimally invasive bone spur removal: Heel spurs or spurs around the ankle can be shaved down through tiny portals without disturbing the surrounding soft tissue.
Neuroma excision: Morton’s neuroma (nerve thickening between toes) can be removed through a tiny dorsal or plantar incision, with most patients recovering in three to four weeks.
Ultrasound-guided wound care: Advanced wound management using ultrasound technology is available locally, combining imaging precision with minimally disruptive treatment. Stride Foot and Ankle is noted for offering ultrasound wound healing therapy, a distinction that few local practices can claim.
Who is performing MIS in Las Vegas?
Several highly rated podiatrists practice MIS in Las Vegas. Local specialists such as Dr. Michael Rossidis (who focuses on MIS and arthroscopy at Nevada Orthopedic), Dr. Thomman Kuruvilla (known for successful bunionectomy outcomes), and Dr. Roger Reed bring strong records and patient ratings between 4.7 and 4.9 out of 5.0.
“Choosing the right foot surgeon in Las Vegas means looking beyond the credential list. Patient reviews, surgical volume, and a surgeon’s willingness to discuss the limits of any given technique are just as important as years of experience.”
What separates the best from the rest is not just technical skill. It is the ability to match the right procedure to the right patient, communicate honestly about expectations, and follow through with attentive postoperative care. When reading reviews, notice whether patients mention how well they were informed before surgery and how quickly the practice responded to concerns afterward.
Pro Tip: Do not rely solely on star ratings. Read the actual written reviews for patterns. Multiple patients mentioning the same surgeon trait, whether positive or concerning, tells you far more than an average score ever could. Also ask about the surgeon’s revision rate and how often they refer complex cases to other specialists.
For patients needing care beyond standard surgical treatment, general foot care services at a quality practice will ensure your entire foot health picture is addressed, not just the surgical component.
How to decide: Is minimally invasive surgery right for you?
Making the decision to pursue surgery is significant. And choosing between MIS and traditional open surgery adds another layer of complexity. Here is a practical framework to help you think it through.
Factors that support MIS as a good option
- Mild to moderate deformity: If your bunion or hammertoe is in early to moderate stages, MIS typically delivers excellent correction
- Younger or middle-aged patients who are active and need to return to normal function quickly
- No significant bone disease or structural irregularities that would complicate the use of small tools
- Strong motivation to minimize downtime, such as patients whose work or family responsibilities do not allow for a lengthy recovery
- No prior surgery on the affected area that might have created scar tissue complicating access through small incisions
Factors that may favor traditional open surgery
- Severe angular deformities where large corrections are needed and require full surgical access
- Significant arthritis involving the joint, which often requires fusion or joint replacement
- Revision surgery from a prior failed procedure
- Complex anatomy or multiple simultaneous deformities in the same foot
Research consistently shows that MIS outcomes benchmarks support faster rehabilitation compared to open procedures for appropriately selected patients, but severe cases need traditional methods for durability and complete correction.
Step-by-step guide: How to evaluate your options
Document your symptoms thoroughly. Note when pain started, what makes it worse, what you have already tried, and how it affects daily activities.
Schedule a diagnostic imaging appointment. Weight-bearing X-rays are essential for assessing deformity severity. Some cases also benefit from MRI or ultrasound.
Consult a specialist who performs both MIS and open surgery. A surgeon who only does one approach may not give you an unbiased recommendation.
Ask specific questions during your consultation (see below).
Get a second opinion for any major procedure. This is especially important if you are a younger patient whose long-term foot health depends on the decision.
Review your recovery timeline against your lifestyle. Be realistic about what you can manage. Rushing back too soon after any foot surgery leads to complications.
Questions to bring to your consultation
- Am I a good candidate for MIS specifically, or would open surgery serve me better?
- What is the expected correction angle for my deformity with each approach?
- What is your personal complication rate for this procedure?
- How many of these procedures have you performed in the past year?
- What does my recovery look like week by week?
- When can I return to walking, driving, and exercise?
Pro Tip: Always bring a printed or digital list of your current medications, past surgeries, and relevant medical history to your consultation. Surgeons who specialize in minimally invasive techniques need complete information to assess whether you are a safe candidate. Do not assume your regular doctor has shared everything that matters. For patients dealing with skin-related foot issues alongside structural problems, resources like treating foot warts and foot fungus treatment options can help you address the full picture of your foot health before surgery.
Our take: Why minimally invasive isn’t always the best choice
Here is something you will not always hear from practices eager to market the latest techniques: minimally invasive surgery is not the right answer for every patient, and pushing it as such does a real disservice to the people we are trying to help.
The enthusiasm around MIS is understandable. The clinical results, especially in hallux valgus correction, are genuinely impressive. MIS benchmarks show faster rehabilitation, significant pain reduction, and high patient satisfaction. But clinical data comes from carefully selected patient populations. In practice, not every patient who walks through the door fits that profile.
We see younger patients in particular who are drawn to MIS because they want to get back to running, hiking, or working on their feet as soon as possible. That instinct is understandable, but if the deformity is severe enough to require a more extensive correction, choosing MIS just to shorten recovery can mean inadequate realignment. That leads to the deformity returning, followed by revision surgery that is harder, riskier, and ultimately more disruptive than the open procedure would have been the first time.
Las Vegas is a city where trends move fast, and the healthcare market is no exception. Some clinics advertise minimally invasive procedures heavily because patients ask for them, not necessarily because the technique is the best match. Our strong advice is this: choose a practice and a surgeon who will tell you honestly when MIS is not the right fit for your case, rather than one who fits your case to the procedure they prefer to perform.
Long-term durability matters enormously, especially for active patients under 50. A procedure that offers a slightly faster initial recovery but fails to provide lasting correction is not a better outcome. When we evaluate patients here in Las Vegas, we consider the full arc of their foot health, not just the six weeks after surgery. Good expert wound care and thorough follow-up are part of that picture.
The most important thing you can do is find a surgeon who thinks the same way: outcome-driven, honest about technique limitations, and focused on what your foot will feel like five years from now, not just five weeks post-op.
Connect with experienced podiatrists in Las Vegas
If reading this has helped clarify what minimally invasive surgery could mean for your situation, the next step is a real conversation with a specialist who can evaluate your specific foot condition.
At Stride Foot and Ankle, we understand that every patient’s foot is different, and we treat it that way. Whether you are dealing with a bunion that has worsened over years, a hammertoe causing daily discomfort, or chronic heel pain that has not responded to conservative care, Dr. Nahad Wassel and our team are here to guide you through every option available. As a trusted podiatrist in Las Vegas, we offer both surgical and nonsurgical approaches, including foot and ankle care options tailored to your activity level, medical history, and goals. We are also proud to offer ultrasound wound healing therapy, one of the few practices in Las Vegas providing this advanced service. Book a consultation today and start striding confidently toward better foot health.
Frequently asked questions
Is minimally invasive foot surgery safe for all patients?
Minimally invasive surgery is generally very safe for most patients, but severe deformities or certain conditions may require traditional open surgery for complete and durable correction. Your surgeon should evaluate your imaging and overall health before recommending any approach.
How long does recovery take after minimally invasive foot surgery?
Recovery is faster than traditional surgery, with many patients experiencing improved pain and mobility within a few weeks. Clinical data shows VAS pain scores dropping from 2.91 to 0.20 post-surgery, indicating near-complete relief for most MIS candidates.
Are Las Vegas podiatrists skilled in minimally invasive techniques?
Yes, Las Vegas has several highly rated specialists in MIS foot surgery. Podiatrists such as Dr. Michael Rossidis, Dr. Thomman Kuruvilla, and Dr. Roger Reed all offer minimally invasive procedures with patient satisfaction ratings between 4.7 and 4.9 out of 5.0.
What conditions are commonly treated with minimally invasive foot surgery?
Common conditions include bunions, hammertoes, plantar fasciitis, neuromas, and bone spurs. MIS techniques are most effective for mild to moderate deformities, with open surgery remaining the standard for complex or severe cases.
Recommended
- General Foot & Ankle Care – Stride Foot & Ankle
- Blog – Stride Foot & Ankle – Dr. Nahad Wassel
- Ingrowing Toenails Can Be Treated – Stride Foot & Ankle – Dr. Nahad Wassel
- Best Podiatrist in Las Vegas | Stride Foot & Ankle
- Why Elevate Your Feet: Relief, Recovery, and Wellness – Lunix
- Top 5 Reasons Mobility and Recovery are Crucial for Active Lifestyles
Recent Comments