Foot pain can stop you in your tracks, and when it does, most people focus on finding a podiatrist who can fix the problem fast. What many patients don’t realize is that two clinics offering the same treatments can produce very different outcomes depending on how care is delivered. Las Vegas practices that emphasize empathy and tailored plans are seeing better results not just in healing times, but in patient satisfaction and long-term quality of life. This guide explains what patient-centered care actually means, what the evidence shows, and how it’s changing podiatry in Las Vegas.
Table of Contents
- What is patient-centered care in podiatry?
- The proven benefits of patient-centered care for foot pain and injuries
- How Las Vegas podiatrists put patient-centered care into practice
- Beyond the basics: Technology, teamwork, and the future of patient-centered podiatry
- A foot forward: The realities and future of true patient-centered podiatry
- Get patient-centered foot care in Las Vegas
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Patient-centered care defined | PCC puts your needs and preferences at the heart of every treatment decision in podiatry. |
| Superior clinical outcomes | PCC leads to better healing, less pain, and lower complication rates for conditions like wounds and diabetic foot. |
| Conservative first approach | Las Vegas podiatrists prioritize non-surgical treatments and tailor plans for best results. |
| Technology with empathy | The best clinics use innovations and teamwork to personalize care, never replacing the human touch. |
| Choose empowered care | Patients should seek providers who involve them in decisions and treat root causes, not just symptoms. |
What is patient-centered care in podiatry?
Now that you know why the approach to care matters, let’s break down what patient-centered care really means in podiatric medicine.
Patient-centered care, often abbreviated as PCC, is a model of healthcare that starts with you, not your diagnosis. Rather than applying a standard protocol to every patient with plantar fasciitis or a diabetic foot wound, a patient-centered podiatrist takes time to understand your specific concerns, goals, lifestyle, and preferences before recommending a path forward. This sounds simple, but it represents a significant shift from traditional “diagnose and treat” medicine.
The core elements of PCC in podiatry include:
- Active listening: Your podiatrist gives you real time to describe your symptoms, history, and concerns without cutting you off.
- Clear explanations: Medical terms are explained in plain language so you understand your diagnosis and why a specific treatment is recommended.
- Shared decision-making: You are included in choosing your treatment path, weighing the pros and cons together with your provider.
- Respect for your experience: Your daily activities, work demands, and pain tolerance are factored into the plan, not ignored.
- Continuity of care: Follow-up appointments track your progress against goals you helped set.
These elements are not just nice to have. Effective communication in podiatry has been shown through empirical evidence to improve diagnoses, increase patient adherence to treatment plans, and produce better overall outcomes. When patients understand what is happening and feel respected, they follow through with exercises, wear their orthotics consistently, and return for follow-up care.
“You should feel heard at every appointment. If your provider is not asking about your goals or explaining your options, that’s a signal the care model may not be truly patient-centered.”
Pro Tip: Before your first podiatry appointment, write down your three biggest concerns and your main goal for treatment. Sharing this list helps your provider understand what matters most to you and sets the stage for a genuinely collaborative visit.
You can explore general foot care options and review treatment plan examples to get a sense of what a patient-centered approach looks like in practice before your first visit.
The proven benefits of patient-centered care for foot pain and injuries
With PCC defined, it helps to see how these principles make a tangible difference. Let’s look at result-driven examples and evidence from clinical settings directly relevant to Las Vegas patients.
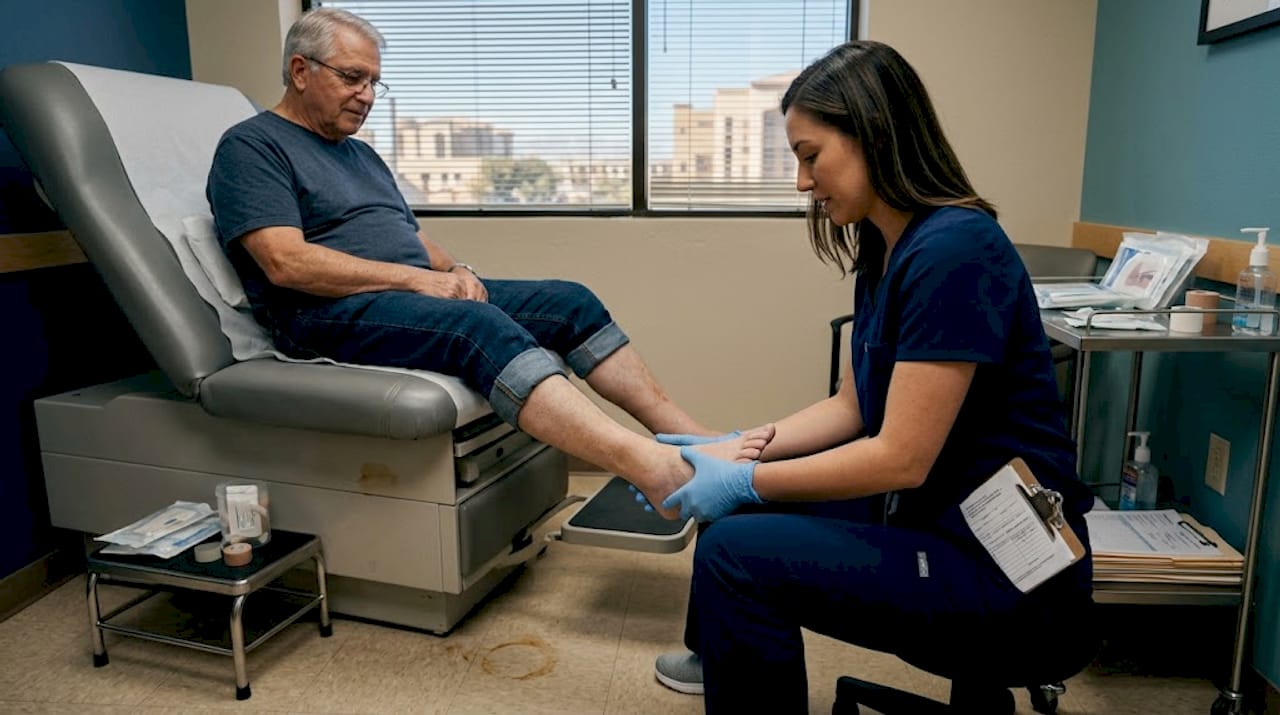
The research on patient-centered care in podiatry is compelling, particularly for patients managing chronic conditions like diabetes or recovering from foot surgery. Studies consistently show that when patients are active participants in their care, outcomes improve across multiple measures including wound healing, pain reduction, and mental health.
Diabetic foot care: a striking example
Diabetic foot ulcers (DFUs) are one of the most serious and costly complications of diabetes. They are also one of the clearest areas where PCC in diabetic foot care demonstrates measurable superiority. By building interdisciplinary teams and actively involving patients in their care decisions, some programs have reduced major amputation rates by up to 75%. That is not a small improvement. That is a life-changing outcome for thousands of patients.
Wound healing outcomes
A clinical study comparing patient-centered wound care to routine wound care produced striking numbers. The PCC wound care group achieved a 40.51% reduction in wound area, compared to just 27.43% in the routine care group, a statistically significant difference (p less than 0.05). Beyond wound size, the PCC group also showed better granulation tissue formation, lower symptom burden, and improved psychological health scores.
| Outcome Measure | Patient-Centered Care | Routine Care |
|---|---|---|
| Wound area reduction | 40.51% | 27.43% |
| Granulation tissue improvement | Significantly better | Moderate |
| Symptom reduction | Greater | Standard |
| Psychological health scores | Improved | Unchanged |
| Patient satisfaction | High | Average |
Post-surgical recovery
For patients recovering from foot and ankle surgery, patient-centered approaches use validated tools like the Foot and Ankle Outcome Score (FAOS) to measure recovery from the patient’s perspective, not just the surgeon’s. This means tracking your ability to perform daily activities, your pain levels during specific movements, and your quality of life, not just whether the incision healed cleanly.
Key benefits documented across PCC studies in podiatry include:
- Faster return to normal activity after surgery
- Lower rates of treatment non-adherence
- Reduced anxiety and depression related to chronic foot conditions
- Greater patient confidence in managing their own foot health
- Higher satisfaction scores across all demographics
Explore wound care options available in Las Vegas if you or someone you know is managing a diabetic foot wound or a slow-healing injury.
How Las Vegas podiatrists put patient-centered care into practice
But how does this look in a real clinical setting? Here’s how Las Vegas clinics are making PCC the norm, not the exception.
Las Vegas podiatrists who practice PCC follow a clear philosophy: treat the root cause, not just the symptom, and always start with the least invasive option. Conservative-first treatment approaches are the foundation, meaning surgery is considered only after non-surgical options have been thoroughly explored and attempted.
Here is a numbered breakdown of how a patient-centered podiatry visit typically unfolds in Las Vegas:
- Comprehensive intake: Your provider spends meaningful time reviewing your full medical history, current medications, lifestyle, and activity level before examining your foot.
- Thorough physical exam: The exam goes beyond the painful area to identify contributing factors like gait abnormalities, muscle weakness, or structural issues.
- Plain-language diagnosis: Your provider explains what is wrong, why it happened, and what the body is doing in response, in terms you can actually understand.
- Collaborative treatment planning: You discuss options together. For most conditions, this starts with conservative care such as custom orthotics, physical therapy, anti-inflammatory treatments, or regenerative medicine options like platelet-rich plasma (PRP) therapy.
- Goal-setting: You and your provider agree on specific, measurable goals, such as being able to walk 30 minutes without pain within eight weeks.
- Follow-up accountability: Progress is tracked at each visit against those goals, and the plan is adjusted if needed.
| Approach | Traditional Podiatry | Patient-Centered Podiatry |
|---|---|---|
| Starting point | Diagnosis and standard protocol | Patient’s goals and concerns |
| Treatment priority | Fastest clinical fix | Conservative options first |
| Patient role | Passive recipient | Active participant |
| Success measure | Clinical markers only | Clinical and quality-of-life markers |
| Communication style | Provider-directed | Shared decision-making |
Many Las Vegas podiatrists also bring personal or athletic experience with injury to their practice. This background builds genuine empathy because your provider understands what it feels like to be sidelined by pain and to work through a recovery process. That shared understanding shapes how care is delivered.
Pro Tip: When choosing a podiatrist in Las Vegas, ask directly: “What is your first approach to treating this condition?” A provider who immediately jumps to surgery without discussing conservative options first may not be practicing a patient-centered model.
If you want to learn about innovative healing options that go beyond standard care, Las Vegas providers are increasingly offering advanced therapies that fit within a conservative-first framework.
Beyond the basics: Technology, teamwork, and the future of patient-centered podiatry
Las Vegas providers are innovating, but patient-centered care is always evolving. Here’s what you should know about technology and teamwork shaping the future of podiatric care.
Interdisciplinary teams
Complex foot conditions, particularly those involving diabetes, vascular disease, or neurological complications, rarely have a single-specialty solution. Interdisciplinary team models that bring together podiatry, vascular surgery, physical therapy, endocrinology, and wound care specialists have been shown to deliver significantly better outcomes for these patients. Each specialist contributes expertise while the patient remains the focus of every decision.
3D-printed orthotics
Custom orthotics have always been a cornerstone of conservative podiatric care, but 3D printing technology is taking personalization to a new level. Rather than relying on foam impressions alone, 3D-printed insoles are fabricated from precise digital scans of your foot, accounting for pressure distribution, gait patterns, and specific anatomical features. This is particularly valuable for older adults and patients with diabetic neuropathy, where standard insoles may not provide adequate protection.

Artificial intelligence in follow-up care
AI tools are beginning to support patient-centered care in meaningful ways. For example, AI-driven programs can personalize post-operative activity dosing, telling patients exactly how much walking or weight-bearing is appropriate each day based on their specific procedure and healing progress. This kind of precision follow-up was previously impossible to deliver at scale.
However, not all technology serves patients equally. EHR systems and AI billing tools can sometimes pull a provider’s attention away from the patient and toward documentation or administrative tasks. When technology is implemented primarily to improve clinic efficiency rather than patient experience, it can actually undermine the human connection that makes PCC effective.
Key considerations when evaluating a tech-forward podiatry practice:
- Does the technology serve your care, or does it primarily serve the clinic’s workflow?
- Is your provider making eye contact and engaging with you, or primarily focused on a screen?
- Are digital tools used to personalize your treatment, or just to speed up processing?
- Do you receive follow-up communication that feels tailored to your case?
“The best technology in a clinic is invisible to the patient. You feel its benefits through better outcomes and more personalized care, not through flashy equipment you never interact with.”
You can learn more about personalized insole technology and how advanced tools are being applied in Las Vegas podiatry practices today.
A foot forward: The realities and future of true patient-centered podiatry
Many clinics in Las Vegas market themselves as patient-centered. The term has become so widely used that it risks losing its meaning. Here’s an honest take on what separates genuine PCC from a polished waiting room and a friendly front desk.
True patient-centered podiatric care is not about having the newest equipment or a five-star Google review average. It is about whether your care is genuinely tailored to your individual needs and whether you are an active participant in every decision. The biggest advantages of PCC are improved healing, less pain, and greater satisfaction, but these results only materialize when care is genuinely interactive and tailored, not when a clinic simply checks boxes on a patient satisfaction survey.
We see patients regularly who come to us after experiences at other practices where they felt rushed, unheard, or handed a generic treatment plan that didn’t account for their job, their activity level, or their personal goals. That is not patient-centered care. That is standard care with a friendlier name.
The uncomfortable truth is that real PCC takes more time. It requires providers who are willing to slow down, ask better questions, and sometimes recommend a less profitable conservative treatment over a surgical procedure that would generate more revenue. It requires a practice culture that values outcomes over throughput.
What should you demand from your podiatrist? Ask for outcome measures. Ask how your progress will be tracked. Ask what happens if the first treatment doesn’t work and what the next step would be. Ask whether your preferences and lifestyle were considered in the recommendation you just received. If you can’t get clear answers to these questions, you may not be receiving true patient-centered care.
The future of podiatry in Las Vegas belongs to practices that combine clinical excellence with genuine human connection. Technology will keep improving. Surgical techniques will keep advancing. But the patients who heal fastest and feel most satisfied will always be the ones whose providers took the time to understand them as individuals.
Get patient-centered foot care in Las Vegas
Ready to take the next step toward pain-free movement? Discover your options for patient-centered podiatric care in Las Vegas.
At Stride Foot & Ankle, patient-centered care is not a marketing phrase. It is the foundation of how Dr. Nahad Wassel approaches every appointment, every diagnosis, and every treatment plan. From custom orthotics and innovative therapies to advanced surgical care when it’s truly needed, the practice combines clinical expertise with a genuine commitment to your goals and quality of life.
Whether you’re managing a diabetic foot wound, recovering from an injury, or dealing with chronic foot pain that’s affecting your daily life, Stride Foot & Ankle offers foot and ankle care options tailored to your specific needs. The practice also provides specialized wound care using advanced techniques that reflect the latest evidence in patient-centered treatment. Schedule your appointment today and experience care that starts with you.
Frequently asked questions
How is patient-centered care different from traditional podiatry?
Patient-centered care puts your needs, goals, and preferences at the center of every decision, rather than applying a one-size-fits-all protocol to your diagnosis. Traditional podiatry tends to follow standard clinical pathways without necessarily accounting for your individual lifestyle or preferences.
Can patient-centered care prevent surgery?
Yes. By prioritizing conservative-first treatment and identifying the root cause of your foot problem, PCC often resolves conditions that might otherwise require surgical intervention. Surgery remains an option when necessary, but it is not the default starting point.
Is patient-centered care effective for diabetic foot wounds?
Absolutely. PCC in diabetic foot care has been shown to reduce major amputation rates by up to 75% and produce significantly better wound healing outcomes compared to routine care models.
What should I look for in a patient-centered podiatrist?
Look for a provider who listens without rushing, explains your diagnosis in plain language, and involves you in choosing your treatment path. Key elements of PCC include active listening, clear communication, and shared decision-making that reflects your personal goals.
Does technology help or harm patient-centered care?
It depends on how it’s used. AI and 3D-printed insoles can genuinely enhance personalized care, but technology focused primarily on billing or administrative efficiency can pull providers away from meaningful patient interaction. The best practices use technology to serve patients, not replace the human connection.
Recent Comments